-
Benzodiazepine Dose Conversion Tools
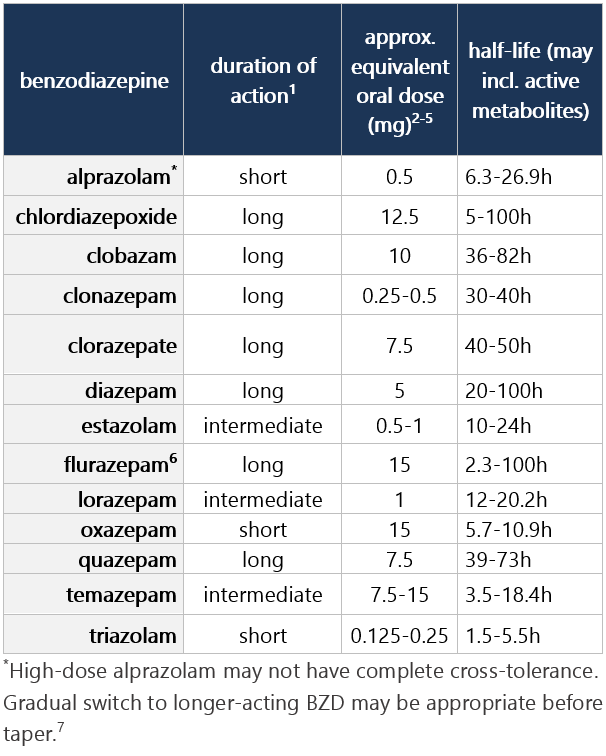
Benzodiazepine oral equivalents table Clinical considerations - Approximate oral dose equivalents and duration of action may vary by resource and don’t account for pt variables (genetics, organ fxn, PK, DDIs, tolerance); refer to monograph and mfr PI for full prescribing info
Benzodiazepine oral equivalents table Footnotes 1 Griffin CE III, et al. Benzodiazepine pharmacology and central nervous system-mediated effects. Ochsner J. 2013 Summer;13(2):214-23. Free full-text PDF in PubMed® Central
• short-acting BZD: average half-life ≤12h
• intermediate-acting BZD: average half-life 12-40h
• long-acting BZD: average half-life ≥40h
2 VA/DoD 2021. VA/DoD Clinical Practice Guideline for the Management of Substance Use Disorders. (Based on evidence reviewed through June 30, 2020.) Version 4.0. U.S. Department of Veterans Affairs. U.S. Department of Defense. August 2021. Free full-text PDF
3 Center for Substance Abuse Treatment. Detoxification and Substance Abuse Treatment. Treatment Improvement Protocol (TIP) Series, No. 45. HHS Publication No. (SMA) 15-4131. Rockville, MD: Center for Substance Abuse Treatment, 2006. Free full-text PDF
4 Borrelli EP, et al. Application of a diazepam milligram equivalency algorithm to assess benzodiazepine dose intensity in Rhode Island in 2018. J Manag Care Spec Pharm. 2022 Jan;28(1):58-68. Free full-text PDF
5 Ashton CH. Benzodiazepines: How They Work and How to Withdraw (aka The Ashton Manual). benzo.org.uk. Updated August 2002. Accessed September 15, 2023
6 Discontinued early 2022; estimated relaunch date December 2023
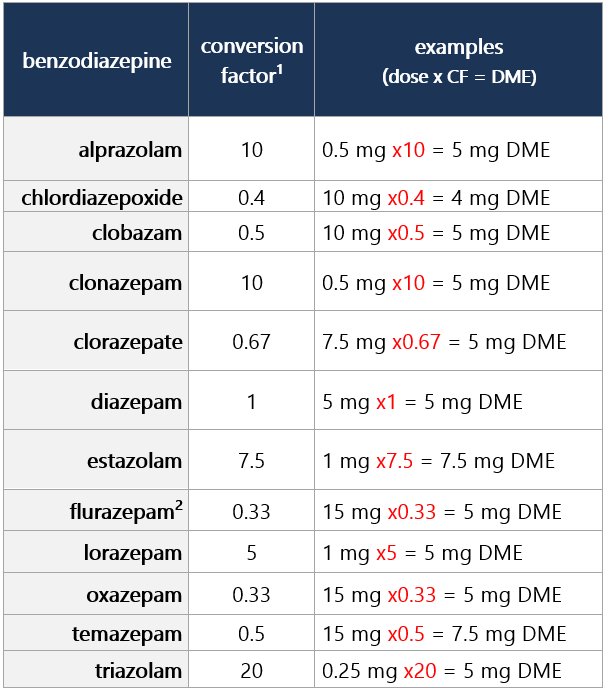
7 VA 2021. Re-evaluating the Use of Benzodiazepines. A Quick Reference Guide. U.S. Department of Veterans Affairs. October 2021. Free full-text PDF Diazepam milligram equivalents (DME) conversion factors table Clinical considerations - Conversion factors apply to oral administration
DME conversion factors table Footnotes 1 Borrelli EP, et al. Application of a diazepam milligram equivalency algorithm to assess benzodiazepine dose intensity in Rhode Island in 2018. J Manag Care Spec Pharm. 2022 Jan;28(1):58-68. Free full-text PDF
2 Discontinued early 2022; estimated relaunch date December 2023 -
Benzodiazepine Deprescribing Advice
Consider deprescribing (tapering and stopping) for any pt >65 yo,1,2 taking BZD >2-4wk,1,3-5 or as appropriate based on pt-specific factors,6 esp. if: - Taking multiple BZDs, BZD w/ opioids or amphetamines, or supratherapeutic dose3-5
- Cognitive d/o, TBI hx, current or hx of substance use d/o, esp. sedative-hypnotic, alcohol, or opioid use d/o3-5
BZD not recommended for long-term mgmt of insomnia or anxiety, PTSD, or w/ opioids outside of palliative care or hospice (i.e., exceptional circumstance)3-5
Footnotes 1 Croke L. Deprescribing Benzodiazepine Receptor Agonists for Insomnia in Adults. Am Fam Physician. 2019 Jan 1;99(1):57-58. Free full-text article
2 AGS 2019. American Geriatrics Society 2019 Updated AGS Beers Criteria® for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc. 2019 Apr;67(4):674-694. PubMed® abstract
3 VA 2015. Effective Treatments for PTSD: Helping Patients Taper from Benzodiazepines. U.S. Department of Veterans Affairs. January 2015. Free full-text PDF
4 Ogbonna CI, et al. Tapering Patients Off of Benzodiazepines. Am Fam Physician. 2017 Nov 1;96(9):606-610. Free full-text article
5 Benzodiazepines: Tapering and Prescribing. Presbyterian Healthcare Services. February 2023. Free full-text PDF
6 Center for Substance Abuse Treatment. Detoxification and Substance Abuse Treatment. Treatment Improvement Protocol (TIP) Series, No. 45. HHS Publication No. (SMA) 15-4131. Rockville, MD: Center for Substance Abuse Treatment, 2006. Free full-text PDF
Engage the pt - Discuss risks of continued BZD use (disinhibition, ineffectiveness, mental acuity loss), benefits of stopping, possible w/d sx, and likely duration1,2
- Assess pt readiness (willing, committed, w/ adequate social support) and suitability (no complicated drug w/d hx) to d/c or ↓ BZD dose1-3
- Assess condition for which BZD originally prescribed; consider alternative tx and/or behavioral services referral as clinically appropriate1-3
- Consider specialist referral if: substance use d/o hx, severe medical or psychiatric d/o, high-dose BZD,4 concurrent stimulant or opioid use, drug w/d sz hx2,3
Individualize gradual taper via shared decision-making;2-6 provide written taper schedule;1,2,7 taper rate determined by w/d sx severity1-3 - Longer taper: ↓ by 10% of original dose no faster than q2-4wk;1,3,7 recommended to prevent severe w/d and aid in BZD d/c;1 longer or high-dose BZD use warrants longer taper1,7
- Shorter taper: ↓ by 10% to 15% of original dose qwk x4wk until 50% of original dose reached, then maintain that dose x1-2mo, then ↓ by 25% of remaining dose q2wk; consider if low-dose BZD use for <1y1
- A more-rapid taper (e.g., ↓ by 25% of original dose qwk) may be appropriate if respiratory depression risk or evidence of misuse/diversion2,3
- Rapid taper of alprazolam or abrupt switching not recommended due to w/d sz risk1-3,7
Follow q1-4wk;2,3,7 monitor for w/d sx and treat symptomatically;2,3,5 pause/slow taper if needed1-3,5-7 - If taper of short-acting BZD intolerable, consider switch to longer-acting BZD (diazepam if <65 yo, lorazepam if ≥65 yo); switch by substituting diazepam or lorazepam for 1 dose of current BZD, starting w/ nighttime dose, then individually replace other doses at intervals of a few days or qwk1,3
- Avoid: ↑ dose or prn use of BZD once taper initiated7
- Any ↓ in BZD use beneficial; if initial attempt unsuccessful, treat underlying conditions and encourage subsequent taper attempt3
- If multiple unsuccessful taper attempts and/or signs of misuse: Consider sedative, hypnotic, or anxiolytic use d/o and/or specialist referral3,6
Footnotes 1 VA 2021. Re-evaluating the Use of Benzodiazepines. A Quick Reference Guide. U.S. Department of Veterans Affairs. October 2021. Free full-text PDF
• Sample tapers available
2 Benzodiazepines: Tapering and Prescribing. Presbyterian Healthcare Services. February 2023. Free full-text PDF
3 Benzodiazepine and Z-Drug Safety Guideline. Kaiser Permanente. January 2022. Free full-text PDF
4 Cloos J-M, et al. Benzodiazepine high-doses: The need for an accurate definition. Int J Methods Psychiatr Res. 2021 Dec;30(4):e1888. Free full-text article in PubMed® Central
• No universally accepted definition of high-dose BZD
5 VA/DoD 2021. VA/DoD Clinical Practice Guideline for the Management of Substance Use Disorders. (Based on evidence reviewed through June 30, 2020.) Version 4.0. U.S. Department of Veterans Affairs. U.S. Department of Defense. August 2021. Free full-text PDF
6 Ogbonna CI, et al. Tapering Patients Off of Benzodiazepines. Am Fam Physician. 2017 Nov 1;96(9):606-610. Free full-text article
7 Gold J, et al. Pharmacist Toolkit: Benzodiazepine Taper. College of Psychiatric and Neurologic Pharmacists (CPNP). 2018. Free full-text PDF
Acute w/d sx may occur w/in 1-7 days, can last 4-14 days after BZD d/c; sx generally more severe but shorter in duration w/ BZD w/ short vs. long half-life1,2 - Mild: anxiety, insomnia
- Moderate: diaphoresis, HA, irritability, muscle pain/stiffness, N/V, palpitations, panic attacks, poor concentration, sleep disturbance, tremor, wt loss
- Severe: sz, psychosis
Nonpharmacologic mgmt1 - Insomnia, nightmares, sleep disturbance: sleep hygiene, relaxation tapes, anxiety mgmt, exercise, BZD scheduled at night during taper
- Anxiety and panic attacks: individual or group behavior tx, CBT, physical activity, yoga, meditation, acupuncture
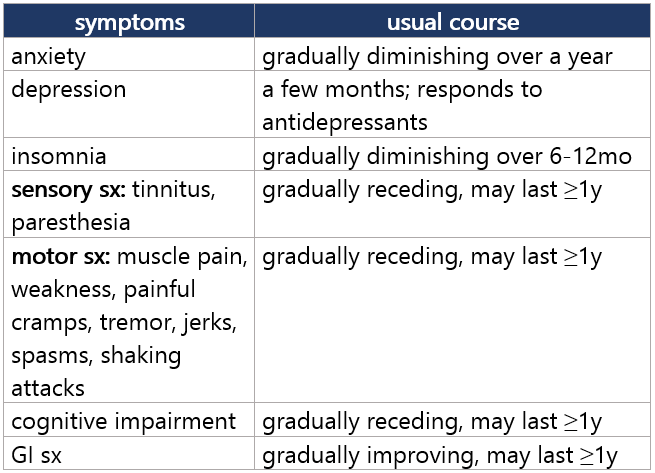
Protracted w/d sx table1,3 Footnotes 1 VA 2021. Re-evaluating the Use of Benzodiazepines. A Quick Reference Guide. U.S. Department of Veterans Affairs. October 2021. Free full-text PDF
2 VA/DoD 2021. VA/DoD Clinical Practice Guideline for the Management of Substance Use Disorders. (Based on evidence reviewed through June 30, 2020.) Version 4.0. U.S. Department of Veterans Affairs. U.S. Department of Defense. August 2021. Free full-text PDF
3 Ashton CH. Benzodiazepines: How They Work and How to Withdraw (aka The Ashton Manual). benzo.org.uk. Updated August 2002. Accessed September 15, 2023
• An estimated 10% to 15% of long-term BZD users will develop protracted w/d sx (i.e., post-acute w/d syndrome) Sedative, hypnotic, or anxiolytic use d/o dx Consider if misuse behavior signs or unanticipated challenges to tapering. If sedative, hypnotic, or anxiolytic use d/o diagnosed, consider specialist referral DSM-51 definition: problematic use w/ clinically significant impairment/distress in a 12-mo period. Mild=2-3, Mod=4-5, Severe=6+ of these: - Often taking larger amounts or over longer period than intended
- Persistent desire or unsuccessful efforts to cut down/control use
- Spending significant time obtaining/using/recovering from substance
- Strong urge to use sedative, hypnotic, or anxiolytic
- Recurrent use interferes w/ work/school/home
- Continued use despite recurrent social/interpersonal problems from substance
- Important activities reduced/given up due to use
- Recurrent use in physically hazardous situations
- Continued use despite recurrent physical/psych problems caused by substance
- Tolerance, defined as 1) need for markedly increased amounts to achieve intoxication/desired effect, or 2) markedly diminished effect using same amount2
- Withdrawal, defined as 1) characteristic sedative, hypnotic, or anxiolytic w/d or 2) using sedative/hypnotic/anxiolytic/related substance to relieve/avoid w/d sx2
Footnotes 1 Cloos J-M, et al. Benzodiazepine high-doses: The need for an accurate definition. Int J Methods Psychiatr Res. 2021 Dec;30(4):e1888. Free full-text article in PubMed® Central
2 Doesn’t apply when taken solely under appropriate medical supervision
|